Medical Imaging Senior Posters showcase innovative research by Misericordia University Medical Imaging winter graduates.
-
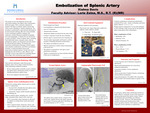
Embolization Of Splenic Artery
Xiahna PM Davis
This project reviews the diagnostic process and intervention leading to the splenic artery embolization (SAE) procedure. SAE is primarily indicated for patients with blunt or traumatic splenic injuries that result in active bleeding or vascular compromise. The procedure is performed by interventional radiologists in an interventional radiology (IR) suite using minimally invasive techniques guided by imaging, most commonly contrast-enhanced computed tomography (CT) and angiography, to accurately identify the site and severity of injury. Causes of splenic injury, including blunt abdominal trauma, iatrogenic injury, and rare spontaneous ruptures, are discussed to provide context for clinical decision-making. The abstract also summarizes embolization techniques, embolic agents used, potential complications, and follow- up strategies necessary to ensure procedural success and preservation of splenic function. Overall, this review highlights the role of SAE as a safe, effective, and minimally invasive intervention for controlling splenic hemorrhage while maintaining organ function.
Keywords: splenic artery embolization, interventional radiology, blunt splenic trauma, minimally invasive procedure, embolization techniques, splenic preservation
-

Magnetic Resonance Imaging-Guided Breast Biopsy
Ainsley Derck
Magnetic resonance imaging (MRI) -guided breast biopsy is a minimally invasive procedure used to obtain tissue samples that look suspicious on a breast MRI. Because MRI has high soft tissue contrast, subtle abnormalities can be detected that may not be seen well in other breast imaging modalities, like mammography or ultrasound. This makes MRI-guided breast biopsy a valuable option in evaluating suspicious breast tissue abnormalities. The MRI-guided breast biopsy uses MR imaging to accurately locate suspicious tissue and perform a minimally invasive biopsy procedure. During the procedure, MRI is used to position a needle in the breast at the location of the desired biopsy site. After checking that the needle is in the correct location, a vacuum-assisted device is utilized to take the sample. Although there are risks like hematoma or infection, the benefits outweigh the risks. Benefits include but are not limited to, brief recovery time, minimally invasive procedure, and less tissue damage than surgical biopsy. As breast cancer remains one of the most common cancers among women, spreading awareness and understanding the use of MRI to guide breast biopsies is important, as it is a valuable method and plays an essential role in diagnosis.
-

Radiation Dose Reduction Strategies in Interventional Radiology
Breanna Fluhr
This project explains the importance of radiation dose reduction in Interventional Radiology (IR) and the strategies that help protect both patients and healthcare staff. General factors that influence exposure, challenges associated with extended fluoroscopy times, sources of scatter radiation, and the role of proper training and protective equipment are discussed. IR procedures often involve long imaging times and complex patient anatomy, which can significantly increase radiation dose if not carefully managed. Traditional safety practices such as pulsed fluoroscopy, last image hold, collimation, increased distance, and appropriate shielding are essential in minimizing unnecessary exposure. New advancements, including patient dose management software, Radiation Dose Structured Reports (RDSR), and automated monitoring systems, offer improved opportunities for measuring and controlling dose levels. Emerging technology such as SepConv++ video frame interpolation also shows strong potential by allowing lower fluoroscopic frame rates while maintaining diagnostic image quality. These developments contribute to safer imaging environments and better outcomes for both patients and staff. Continual research, education, and quality assurance highlight the ongoing need to refine dose optimization methods in IR.
Keywords: interventional radiology, fluoroscopy, scatter radiation, collimation, ALARA, artificial intelligence
-

Utilizing Shockwave Therapy for Cardiac Catheterization
Nadja E. Hartmann
Abstract
This project explores the role of cardiac catheterization and the use of intravascular shockwave therapy (IVL) in diagnosing and treating coronary artery disease (CAD). Cardiac catheterization is a minimally invasive procedure that allows doctors to visualize coronary and peripheral vessels, assess heart function, and intervene on obstructed arteries. The poster outlines the fundamental steps of catheterization, including the use of specialized catheters, contrast imaging, and tools such as balloons and stents to restore blood flow. The main topic of this project is Shockwave therapy, a newer technique designed to treat heavily calcified lesions that are resistant to other methods, such as atherectomy. Interventional shockwave therapy (IVL) uses high-frequency ultrasonic waves to disrupt calcium within the vessel wall while increasing lumen area, allowing for safer and more effective stent deployment. This project highlights the benefits of shockwave therapy like minimal vessel injury, improved procedural outcomes, and enhanced safety for high-risk patients. Limitations such as device failure, limited long-term research, and rare complications are also addressed. Successful outcomes from recent studies demonstrate promising results, including improved lumen size and reduced restenosis rates. Overall, this project emphasizes how advanced cardiac catheterization procedures, like interventional shockwave lithotripsy (IVL), are reshaping cardiac catheterization and improving treatment options for patients with complex coronary artery disease (CAD).
Keywords: cardiac, catheterization, therapy, coronary artery disease, catheter, Shockwave
-
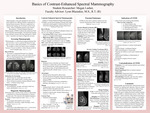
Basics of Contrast-Enhanced Spectral Mammography
Megan A. Lasher
Contrast-Enhanced Spectral Mammography (CESM) is an advanced diagnostic technique that combines anatomical and functional breast imaging with the use of iodinated contrast to enhance potential malignant lesion visualization. This capstone presents the fundamental principles of mammography, clinical indications and contraindications, and diagnostic capabilities of CESM compared to traditional mammography. CESM has improved the detection of malignancies, especially in dense breast tissue, as contrast highlights vascular changes associated with tumor angiogenesis. The imaging involves a dual-energy image acquisition, as low-energy is required for structure and high-energy for contrast enhancement. The dual imaging provides a thorough insight into lesion morphology and perfusion. Research shows that CESM offers diagnostic accuracy comparable to Magnetic Resonance Imaging while being faster, more cost-effective, and accessible. However, some contraindications limit patient eligibility, such as, pregnancy, severe allergies, and renal impairment due to contrast-related risks. Overall, the implications of CESM is important and has a growing role in the early detection, staging, and treatment of breast cancer. Furthermore, some future advancements in CESM would be standardizing imaging protocols, potentially expanding CESM to screenings, and increasing the use of CESM in stereotactic biopsies.
Keywords: contrast-enhanced spectral mammography (CESM), contrast-enhanced digital mammography (CEDM), breast cancer, mammography, screening mammogram, diagnostic mammogram, iodinated contrast media, angiogenesis, dense breast tissue, contraindications, indications, invasive ductal carcinoma (IDC), invasive lobular carcinoma (ILC), ductal carcinoma in situ (DCIS), benign findings, cysts, fibroadenomas, enhancement
-
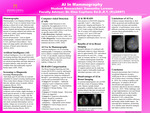
AI in Mammography
Samantha Lorenzo and Gina Capitano
Abstract
This Research explores the benefits of artificial intelligence (AI) in mammography and its role in cancer diagnosis. It examines statistical data related to AI-assisted diagnostics, highlights AI’s ability to detect early signs of cancer that may be imperceptible to the human eye, and discusses the growing adoption of AI among breast radiologists. Breast cancer is the most common cancer among women in the United States and the second-leading cause of cancer-related death. Approximately one in eight women will develop invasive breast cancer during their lifetime. The integration of AI in mammography represents a promising advancement in early detection and diagnostic accuracy. AI-based triage tools can help prioritize patients and enhance workflow efficiency for radiologists interpreting breast imaging studies. AI-powered computer-aided detection (AI-CAD) offers a new and effective approach to identifying breast cancer, potentially reducing its prevalence. Given the high percentage of missed diagnoses in annual screening mammograms, AI presents a valuable opportunity for improving outcomes in breast cancer detection.
-

Radiation Dose in Computed Tomography (CT)
Helen Minnick
Computed Tomography (CT) is a critical diagnostic tool that delivers rapid, detailed cross-sectional imaging but remains a major contributor to medical radiation exposure. Increasing use of CT has led to concerns about excessive or low-value exams, including repeat scans that do not often change patient management and may increase long-term cancer risk. Evidence shows that only a small percentage of repeat head CTs reveal clinically significant findings, underscoring the importance of justification and reducing unnecessary imaging. Pediatric patients are particularly vulnerable due to increased tissue radiosensitivity and longer lifespans, making dose optimization essential. National initiatives such as Image Gently and Image Wisely support radiation safety by promoting the As Low As Reasonably Achievable (ALARA) principle, standardized protocols, automatic exposure control, iterative reconstruction, and clinical decision rules such as the Pediatric Emergency Care Applied Research Network (PECARN) guidelines. These evidence-based strategies maintain diagnostic quality while minimizing exposure. This project reviews current research on CT overuse and dose optimization, highlights best practices for reducing cumulative radiation risk, and emphasizes the need for continued education, collaboration, and adherence to evidence-based guidelines. Future work should explore the long-term outcomes of dose-reduction technologies and evaluate strategies to improve provider decision-making regarding CT use.
-

Magnetic Resonance Imaging Safety and Considerations
Lauren Mosier
Abstract
Magnetic Resonance Imaging (MRI) is considered to be a safe, non-invasive diagnostic modality. However, the presence of a strong magnetic field creates inherent risks when safety protocols are not followed. This project examines MRI safety, with particular focus on the recent fatality in New York, where a person was killed by a projectile accident in the scanner room. Such events highlight the catastrophic consequences that can result from lapses in screening procedures, inadequate staff training, or poor enforcement of zone protocols. By reviewing this incident in the context of MRI safety protocols, this project emphasizes the ongoing need for rigorous adherence to safety standards set forth by organizations such as the American College of Radiology (ACR) and The Joint Commission. The findings suggest that despite technological advancements and well-established guidelines, human error and system failure remain significant contributors to preventable harm. Future practice should include strengthening interdisciplinary education for all personnel entering MRI environments, implementing stricter safety protocols, and prioritizing staff adherence to safety protocols to minimize risk. Ultimately, this project reiterates that MRI safety must remain a top priority to protect patients, staff, and visitors from potentially life-threatening accidents.
-
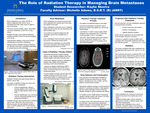
The Role of Radiation Therapy in Managing Brain Metastases
Kaylie Skovira
This project explores brain metastases and the critical role of radiation therapy in managing this condition. It provides an overview of general statistics, radiation therapy types, treatment options, expected outcome and prognosis. Brain metastases rank as the tenth major leading cause of death among men and women, and occur in 20-40% of patients diagnosed with cancer. Radiation therapy for brain metastases primarily involves external radiotherapy, which delivers ionizing radiation from outside of the body to targeted brain regions. Internal radiotherapy is less commonly used due to anatomical constraints.Common treatment options include: CyberKnife stereotactic radiation therapy, whole-brain radiation therapy, intensity-modulated radiotherapy, and focused radiation therapy. Selection of treatment depends on individual patient status and tumor progression. Prognosis varies significantly; patients in good overall condition generally experience better survival outcomes compared to those with declining health.
-
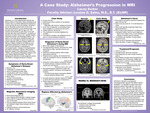
A Case Study: Alzheimer’s Progression in MRI
Lacey E. Sorber
Alzheimer’s is a neurodegenerative disorder that affects millions of Americans. Many individuals know a person who is currently suffering from Alzheimer’s or has lost their life due to the disease. Alzheimer’s can be described as early-onset or late-onset. Early-onset Alzheimer's occurs before the age of 65, and late-onset occurs after the age of 65. This research demonstrates a case study of a 63 year old male with early-onset Alzheimer’s. Symptoms of Alzheimer’s include memory loss, cognitive decline, behavioral changes, and language problems. The patient in this case study’s symptoms began with memory loss and began to regress into cognitive decline. Magnetic resonance imaging (MRI) is an effective imaging modality for the diagnosis and progression assessment of Alzheimer’s disease. MRI is the gold standard in evaluating the neurological system. Changes in the hippocampus are linked to Alzheimer’s disease. MRI provides diagnostic images of the hippocampus of the brain. Thereby, demonstrating pathological changes in the brain making diagnosis possible. This case highlights the importance of early diagnosis and the role of MRI in managing Alzheimer’s disease.
-

Cardiac Catheterization: Percutaneous Coronary Intervention vs Coronary Artery Bypass Grafting
Ethan Sparrow
Abstract
Coronary artery bypass grafting (CABG) and percutaneous coronary intervention (PCI) are the two primary revascularization options for patients with coronary artery disease (CAD). Although advances in PCI technology have led to improved outcomes and increased survival rates, CABG continues to be the preferred option for many patients due to its favorable long-term outcomes. This project examines the key differences between CABG and PCI, including their indications, contraindications, and clinical applications. Quality of life data indicate early benefits with PCI but more sustained improvement with CABG, especially beyond the first year. Findings from the SYNTAX study highlight that PCI is appropriate for patients with uncomplicated left main disease, whereas CABG demonstrates superior outcomes when disease burden is extensive. Technological advancements, including improved stent designs, fractional flow reserve (FFR), and intravascular ultrasound (IVUS), have enhanced PCI results but have not eliminated CABG’s advantages in high-risk cases.
Keywords: CABG, PCI, coronary artery disease, revascularization, SYNTAX score, quality of life, cardiovascular interventions
-

Surface-Guided Radiation Therapy for Treatment of Various Cancers
Taylor J. Windheim
Surface-Guided Radiation Therapy (SGRT) is a newly advancing technology in radiation therapy that improves the accuracy and safety of radiation therapy treatments. SGRT utilizes three-dimensional images of the patient’s surface in real-time, which improves patient setup accuracy and allows for continuous patient monitoring, while decreasing the need for additional imaging in comparison to the traditional laser setup method. The project discusses the advantages of SGRT and the utilization of the technology for breast and lung radiation treatments. In breast cancer treatments, SGRT improves positioning accuracy and reproducibility, as well as decreases radiation dose to the heart and lungs while using deep inspiration breath hold (DIBH). In lung cancer treatments, SGRT decreases setup errors, radiation dose to the patient and treatment time, as well as improves reproducibility of respiratory motion. Additional benefits of the utilization of SGRT includes the elimination of the need for permanent skin marks, reduced close contact between patients and radiation therapists, which decreases disease transmission, and easier setup for radiation therapists compared to conventional setup methods. Overall, SGRT demonstrates a highly advancing technology in radiation oncology, which improves treatment efficiency and accuracy. As SGRT continues to evolve, the technology is expected to become more common in the radiation therapy field; however since SGRT is a new technology, further research is needed to assess the long-term effectiveness.
-
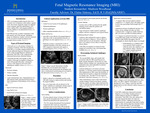
Fetal Magnetic Resonance Imaging (MRI)
Madison Woodhead
This project explains fetal magnetic resonance imaging (MRI) and its role in prenatal diagnosis. It discusses various aspects, including types of prenatal imaging, clinical applications, the imaging procedures, safety considerations, and technical challenges. Understanding the benefits and limitations of fetal MRI allows for earlier and more accurate detection of fetal abnormalities. Fetal MRI serves as a secondary imaging modality that complements ultrasound by providing detailed imaging of fetal anatomy. Several congenital anomalies including those involving the central nervous system (CNS), as well as the abdominal and thoracic regions, can be thoroughly evaluated to provide additional information and confirm diagnoses made using ultrasound. Safety concerns such as tissue heating, acoustic damage, and contrast agent use are evaluated toensure no harm to the fetus. Advances in artificial intelligence (AI) and the use of 3 T scanners over 1.5 T have significantly improved image resolution and reduced motion artifacts. Overall, fetal MRI is improving prenatal diagnosis through ongoing technological advancements.
-
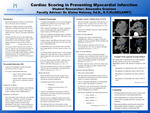
Cardiac Scoring in Preventing Myocardial Infarction
Alexandra Graziano
Abstract
Myocardial Infarctions (MI) occur due to blocked blood flow to the heart, causing damage or death of heart muscle tissue. Men experience MI’s more frequently than women and often show classic symptoms such as chest pain, while women may have less typical signs, such as neck or jaw discomfort, which can lead to delayed medical attention. The Coronary Artery Calcium Score (CACS) is a non-invasive computed tomography exam that measures calcium deposits in the coronary arteries, helping assess the risk of heart disease in individuals with moderate cardiovascular risk. The most common scoring methods include the Agatston Score, Volume Score, and the Mass Score. The Agatston Score is used most frequently because it evaluates both the density and area of calcified plaques. The Volume Score offers reduced sensitivity to noise but with the chance of this overestimating the calcification. The final method, Mass Scoring, considers the amount of calcification along with water and x-ray absorption to try and calculate the score based off mineral mass. Early detection of coronary calcium can support heart disease prevention and improve patients’ outcomes by promoting timely diagnosis and treatment.
Keywords: myocardial infarction, prevention, computed tomography, coronary artery calcium score
-

The Utilization of Radiation Therapy for Benign Pathologies
Chloe Hanselman
This research addressed how radiation therapy can be utilized to treat not only malignancies, but also benign pathologies. Radiation therapy utilizes high-energy radiation in the forms of x-rays, gamma rays, neutrons, protons, and other sources aimed at a precise point in the body to kill unwanted cells and shrink tumors. Treatment plans are created and are unique to every patient. Special equipment like a gamma knife, electron beam, stereotactic radiosurgery, or even proton therapy are selected based on patient condition and tumor location. A benign pathology consists of localized growths that provide low potential for progression. The most common pathologies treated using radiation therapy include meningiomas, eczema, keloid scars, schwannomas, and plantar fasciitis. Radiation therapy treatments for benign tumors are not as common, but are typically used when the area is difficult to reach or surgery has a higher risk for complications. Patients typically seek the anti-inflammatory effects that come from radiation therapy for benign pathologies.
-
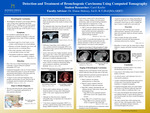
Detection and Treatment of Bronchogenic Carcinoma Using Computed Tomography
Carol Keefer
This project explains bronchogenic carcinoma and the role that computed tomography plays throughout the process, from initial detection through treatment. General statistics, symptoms, steps to obtain diagnosis, and staging of the cancer are discussed as well. Bronchogenic carcinoma is the leading cause of death globally, accounting for 32% in males and 25% in females between the ages of 40-70 years. Over 2.2 million new lung cancer cases were documented globally in 2020 alone, with a survival rate of only 27%. While this fact is frightening, computed tomography has the power to discover potential cancerous lung lesions early on, allowing for a potentially better prognosis for patients. In addition, computed tomography is also used in the biopsy process, as well as during radiation therapy treatments and exams used to check potential metastases of the disease. As technology used in computed tomography advances, this field may lead to more optimistic prognoses for cancer patients worldwide.
-
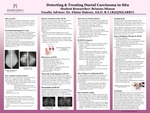
Detecting & Treating Ductal Carcinoma in Situ
Brianna Misson
Mammography is a crucial imaging technique for the early detection of breast cancer, utilizing low-energy X-rays to identify changes in breast tissue that may indicate malignancy. The American College of Radiology and the Society of Breast Imaging suggest annual mammograms starting at age 40, significantly improving outcomes such as mortality reduction and earlier diagnosis. In the U.S., breast cancer remains the most common cancer among women, with approximately 310,720 new invasive cases projected in 2024 and an estimated 42,250 fatalities. Ductal carcinoma in situ (DCIS), a non-invasive type of breast cancer, is seen as a precursor to invasive cancer, detectable through mammography via calcifications, often without symptoms. Risk factors for DCIS include a family history of breast cancer, delayed menopause, and genetic mutations such as BReast CAncer gene 1 (BRCA1) and BReast CAncer gene 2 (BRCA2). Accurate diagnosis typically involves mammographic evaluations categorized using the Breast Imaging Reporting and Data System (BI-RADS) system, followed by biopsies when necessary. Treatment for DCIS often begins with surgical options such as lumpectomy, followed by radiation therapy to reduce recurrence risks. Radiation therapy plays an important role in the treatment of DCIS. Genetic testing and proper follow-up care further enhance management, emphasizing the need for personalized treatment strategies in addressing this prevalent disease.
-

MRI Linear Based Treatment in Radiation Therapy
Sara Mulea
Abstract
This research project explains radiation therapy playing an essential role in cancer treatment, utilizing advanced technology to target and destroy cancerous cells with precision. Central to this process is the linear accelerator, a sophisticated device that emits high-energy radiation and electrons to treat cancerous tissues effectively. Notably, recent technological innovations have led to the development of a new class of linear accelerators integrated with magnetic resonance imaging (MRI), known as MRI-guided linear accelerators (MRgRT). This technology allows clinicians to obtain high-resolution, cross-sectional images of soft tissues in real-time, significantly improving the accuracy of radiation delivery. As a result, MRgRT enables more precise targeting of complex and advanced tumors, minimizing exposure to surrounding healthy tissues and enhancing treatment outcomes.The benefits of MRgRT technology offer increased tumor control rates and reduced side effects, ultimately contributing to better patient outcomes. However, the adoption of MRgRT does face limitations such as the limited availability of this technology and the need for specialized training for healthcare professionals that need addressing. Nevertheless, ongoing research and development efforts aim to overcome these hurdles, making this innovative treatment more accessible. Looking ahead, continuous advancements in MRgRT are expected to broaden its application, allowing for even more personalized cancer care. By providing more accurate and less invasive treatment options, MRgRT holds the promise of significantly improving survival rates and quality of life for cancer patients, paving the way for a future where recovery and long-term health are more attainable.
Keywords: radiation therapy, cancer treatment, MRI machinery
-

Transarterial Chemoembolization in Interventional Radiology
Alexis Pelchar
This project details specifics regarding hepatocellular carcinoma and transarterial chemoembolization. Transarterial embolization involves treatment of liver cancer via arterial access. This procedure is the first line of treatment for individuals diagnosed with stage B hepatocellular carcinoma. Indications, contraindications, procedural aspects, and current research are also discussed. Hepatocellular carcinoma is the fifth leading cause of cancer around the world. The TACE procedure can be done using drug eluting beads to embolize or with the use of chemotherapy drugs. The procedure is credited with extending the life span for individuals with this diagnosis. Research shows the procedure has a positive success rate including a complete response to the procedure in 35% of patients and a reduction of tumor in 25% of patients. Side effects of the procedure are minimal, with most side effects being moderate and treatable. Hepatocellular carcinoma was the third leading cause of death in 2020, which emphasizes the need for understanding and implementation of this procedure.
-

Pediatric Sedation in Computed Tomography Scans
Janelle Smith
This senior capstone project explains the use of pediatric sedatives to acquire Computed Tomography (CT) images of diagnostic quality. Stages and types of pediatric sedatives, risk versus benefit, pros and cons, potential side effects, parental/guardian consent, general statistics, administration and monitoring requirements, indications and contraindications, and an example of motion artifact are also discussed. Sedatives are essential when pediatric patients are anxious and restless prior to receiving a CT scan. The failure rate of acquiring a diagnostic image while using sedatives for pediatric patients has been indicated as 1 to 3% and 10 to 20% through different conducted studies. Parental/guardian consent is important to obtain due to the potential side effects of pediatric sedatives, as it ensures that caregivers are fully informed about risks and benefits, allowing them to make the best decision for the safety and health of the child. Not all forms of pediatric sedation are pharmaceutical, some include non-pharmaceutical methods. The use of pediatric sedation reduces stress and allows for an accurate diagnosis.
-
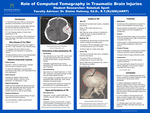
Role of Computed Tomography in Traumatic Brain Injuries
Rebekah Spott
This project explains the role of computed tomography (CT) in assessing traumatic brain injuries (TBI). The major components of the research include various intracranial traumas, penetrating vs. non-penetrating TBIs, symptoms, grades of injury, and treatment options. CT is essential in diagnosing a TBI because it can quickly produce hundreds of images of the brain and skull in slices. CT allows radiologists, physicians, and surgeons to plan a course of action for the best possible patient recovery outcome. Images can identify various lesions and fractures as well as their severity. A TBI can present itself as penetrating or non-penetrating, ultimately determining the type of treatment the patient will receive. The symptoms of a TBI will differ depending on whether the injury is mild, moderate, or severe. Depending on how severe the injury is, a patient may require open or closed brain surgery to remove the damaged brain matter caused by the injury. Overall, a CT scan of the brain for patients who suffered a TBI allows healthcare professionals to determine what can be done to ensure the best outcome for recovery.
-
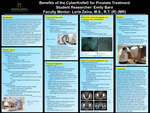
Benefits of the CyberKnife for Prostate Treatment
Emily Baro
Radiation therapy is a type of cancer treatment that uses high- energy rays to kill cancer cells. There are a lot of cancers that can be treated with radiation, but a common type is prostate cancer. Prostate cancer is the most common type of cancer diagnosed in men. The types of radiation therapy used to treat prostate cancer are external beam radiation, brachytherapy, and radiopharmaceuticals. The most common machine used for radiation treatment is the linear accelerator. Most patients are treated using the linear accelerator but a select few can be treated using the cyber knife. The cyber knife is a machine that uses external beam radiation that can treat prostate cancer in qualified patients. Some of the benefits of the cyber knife treatment could be fewer side effects, less radiation to normal tissue and increased accuracy of treatment area compared to traditional radiation treatment. The patients who do not qualify for the cyber knife treatment will be treated using the linear accelerator which will be just as effective.
-

Importance of Deep Inspiration Breath Hold for Left Breast Cancer Treatment
Cassandra Benderavich and Elaine Halesey
Abstract
This project explains the importance of deep inspiration breath hold (DIBH) technique for treating left breast and chest wall tumors. General statistics, definition of gating and DIBH, inclusion and exclusion criteria, dose reduction, differences of free breathing and DIBH techniques, and expected outcome are also discussed. Breast cancer is the leading cause of female deaths in the United States, and left breast cancer diagnosis is more common than right breast cancer diagnosis. Left breast cancer diagnosis accounts for 50.8% of breast cancer diagnosis and right breast cancer accounts for the remaining 49.2%. The risk of breast cancer diagnosis in a female's lifetime is about 1 in 3 women. Radiation therapy utilizes techniques to help alleviate pain and can cure breast cancer cases. New radiation therapy techniques, such as the DIBH, offer greater potential for dose reduction and protection of vital organs from overexposure. Deep inspiration breath hold increases optimism for female patients with left breast cancer due to the reduction in chest wall complications and reactions from therapy treatments. Due to the prevalence of left breast cancer diagnosis, further research needs to be conducted to improve proper treatment and deep inspiration breath hold technique.
Keywords: deep inspiration breath hold, free breathing, breast cancer, left breast cancer, radiation therapy
-

Transcatheter Aortic Valve Replacement (TAVR)
Jocelyn Bergener
Transcatheter aortic valve replacement (TAVR) is becoming the gold standard when repairing aortic stenosis compared to surgical aortic valve replacement (SAVR). Transcatheter aortic valve replacement is minimally invasive. Aortic stenosis is the most common valvular disease in the United States, commonly seen in the elderly population. In this project, multi-imaging modalities are discussed when preparing a patient for TAVR such as computed tomography, left heart catheterization, and transthoracic echocardiography. Each imaging modality has its own specialty in the preprocedural planning of a valve replacement. Computed tomography uses 3D reconstruction to determine the type of valve and size needed for the patient. Transthoracic echocardiography evaluates the severity of aortic stenosis along with the morphologic classification. Left heart catheterizations can determine the severity of aortic stenosis by measuring pressure gradients between the aorta and left ventricle. Patients who undergo transcatheter aortic valve replacement experience a better quality of life, and less major complications when compared to surgical aortic valve replacement (SAVR). Keywords: Transcatheter aortic valve replacement, aortic stenosis, multi-imaging modalities, surgical aortic valve replacement
-

Artificial Intelligence in Computed Tomography
Cheyenne Dippre
Abstract
This research project explains the fundamentals of artificial intelligence (AI) and the ways that AI can be useful in computed tomography (CT). The current state of AI application in CT is still new yet has been advancing with its significant impact on diagnosis, image analyses and patient care. These impacts deal with the challenges that have traditionally been associated with CT scans through a series of techniques and algorithms. In CT, computed tomography angiography (CTA) is a common procedure which is used to diagnose cardiovascular disease (CVD), the leading cause of death worldwide. AI can assist with such a procedure by assessing the degree of stenosis, coronary calcification, and plaque morphology which may prompt a cardiovascular episode. AI systems are capable of rapidly and accurately analyzing CT and CTA scans, assisting radiologists in detecting anomalies and enhancing diagnostic accuracy. Moreover, the AI automation of routine tasks such as organ segmentation and image reconstruction has improved workflow, reduced radiologist fatigue and improved turnaround report times. The process of machine learning (ML) and deep learning (DL) along with their contribution to the healthcare diagnostic process is also discussed. AI in the assistance of chest diagnostics as well as oncological applications are other aspects pertaining to the future of AI in the radiologic setting.While this technology is impressive, there are limitations and misconceptions surrounding the implementation of AI in such a healthcare dynamic.
Keywords: artificial intelligence, computed tomography, cardiovascular disease, computed tomography angiography

